#5 WHAT CHEMOTHERAPY LOOKED LIKE
Chemotherapy is a type of cancer treatment that uses one or more anti-cancer drugs as part of a standardized chemotherapy regimen. It is administered either through an IV or a port. Administering it through a port is a lot easier because the port allows for a needle to be inserted through it with little or no pain. Whereas it is harder on the veins if an IV is used in the arm each time.
My chemotherapy was administered through a port. About an hour before, I applied numbing cream. I then covered it with a protective plastic so it would not get all over my clothes.

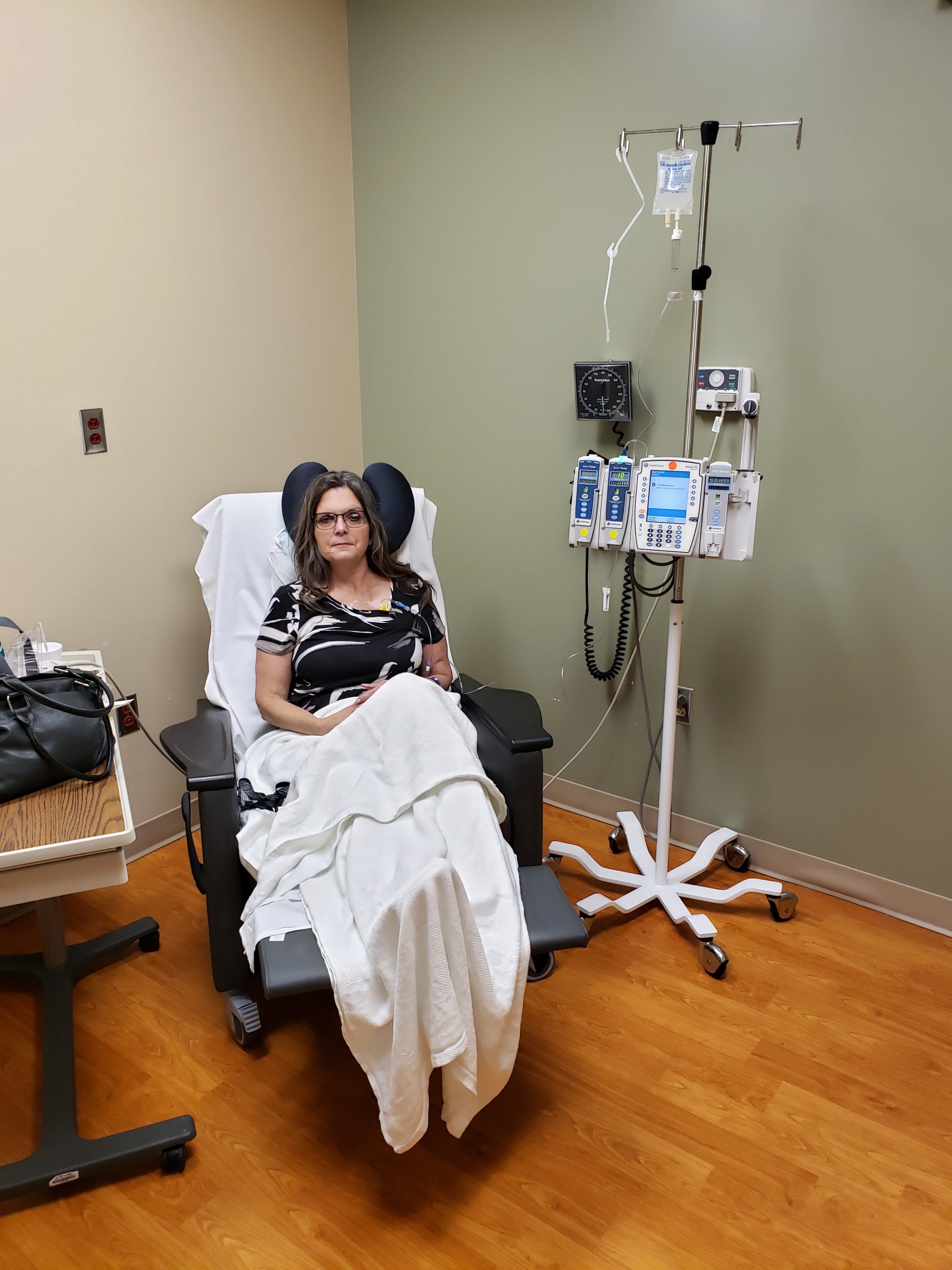
When I got to the chemotherapy area of the hospital, I was assigned a specific chemotherapy room. The nurse took my blood pressure and checked my pulse. Using a stethoscope, she listened to my back and chest as well as my intestine area to make sure all sounded well. Then through her computer, she ordered my chemotherapy prescription from the hospital pharmacy. We waited until it was delivered. In the meantime, the nurse removed the plastic protecting the numbed area. She wiped it off and cleaned the area very well.

This picture shows the needle that the nurse inserted into the port along with a tube that she attached to it.

Here the nurse inserted the needle into the port.

After she inserted the needle, she checked to make sure the port functioned properly. Then she flushed heparin through the port, which helped prevent clotting. If the port was not used for a period of time, I had to make sure that it was flushed approximately every 4 weeks.

The nurse also put clear plastic adhesive over the needle and some of the tubing to hold it in place.

Once the chemo drugs arrived from the pharmacy, the nurse hooked them up to the IV in the order and dose prescribed. Before she administered it, another nurse always verified with the computer the exact dose of the prescription and verified that the prescription going into the port was correct.
Because body temperature changed while the chemotherapy was administered, they offer a heated blanket. I reclined in the recliner and covered up with the blanket. It really added comfort.

Depending on the time of day, they offered a sandwich, chips, and a drink. If it was not during the lunch time, they just offered chips and a drink. I found in the beginning that sometimes the heparin left a weird taste in my mouth. Therefore, the salt from the potato chips helped remove the weird taste. I was also grateful while I ate, that I could take my face mask off.

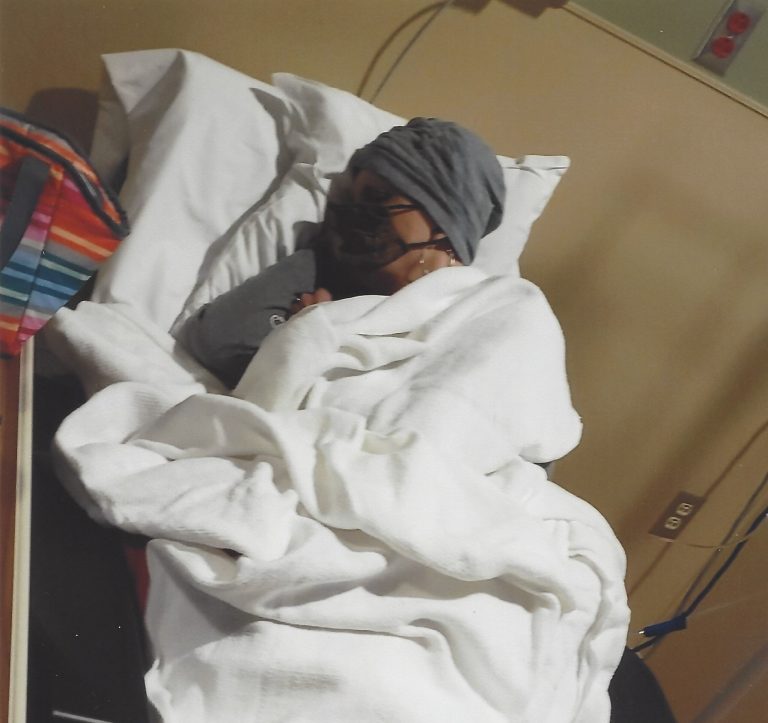
Sometimes, they gave pre-meds before the chemotherapy such as steroids or Benadryl which helped prevent reactions to chemotherapy. When I was given Benadryl within a few minutes, I was extremely tired. As a result, I cuddled up in the recliner and tried to take a nap. Sometimes, it made me so groggy that I had a difficult time putting thoughts together to have a conversation. Because Benadryl really made me tired, I had to have someone drive me home after chemotherapy.
Because I always drove myself from work to the hospital, it caused a conflict when I needed a ride home. We arranged for my mom to drive my husband to the hospital about the time I was done. Then my husband drove me home in my car.
During my first few months of chemotherapy, I was allowed one person with me during the procedure. That always brought me comfort. However, as the months passed and COVID-19 got worse, they restricted visitors. So, I would watch a TV show on my phone to try to distract me when I was not resting.

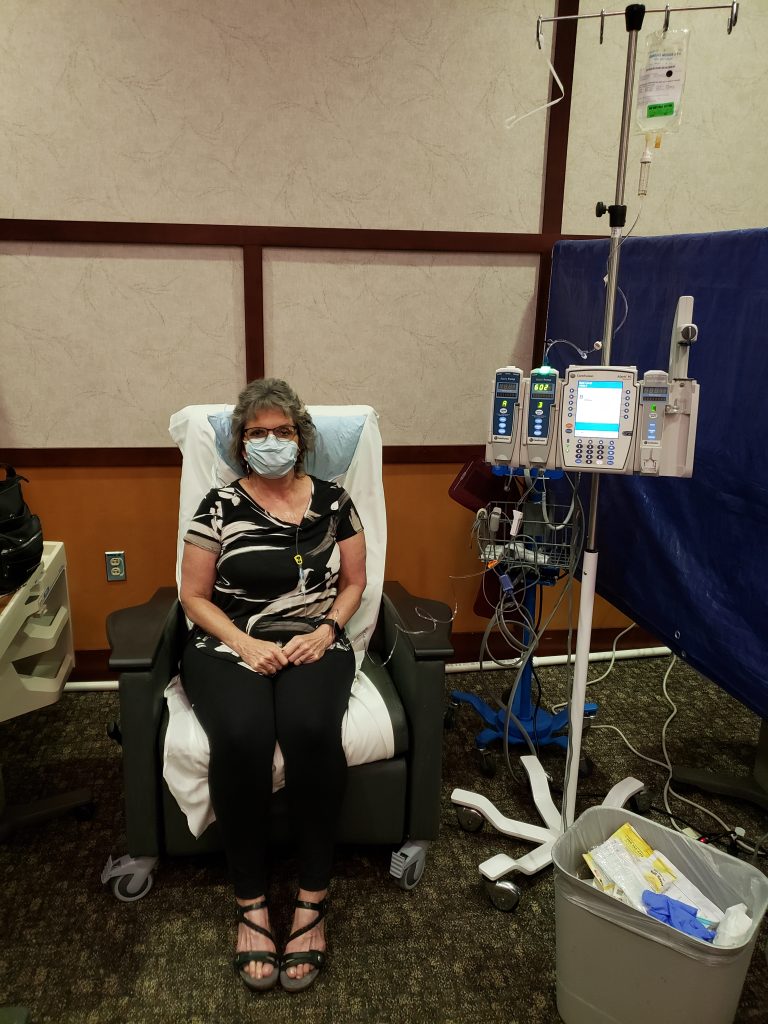
During the height of COVID-19, the chemotherapy area was converted into hospital bed overflow. As a result, the chemotherapy area was moved a couple times to temporary areas. The next picture shows how they made wall supports with PVC and covered them with tarps. One of the nurses said she felt like she was working in a war zone medical area. The nurses made the change work as well as possible, but it was difficult. It was harder for the patients too because there was not as much privacy. Because the dividers did not go to the ceiling like the walls in the chemotherapy original area, noise carried a lot further. Therefore, the area was a lot noisier. The noise made the anxiety of some of the patients worse.
Depending on the type of chemotherapy administered and how it affected the blood levels, Neulasta was given. I was given Neulasta after my first four chemotherapy treatments. It helped build up the bone marrow which in turn helped improve blood levels. Insurance chose to have the Neulasta administered through this devise on the back side of my arm instead of a shot. After the chemotherapy was administered, the nurse attached the Neulasta to the arm with the adhesive. Within a couple minutes I heard a beeping sound. Then it automatically inserted a needle into my arm. It barely hurt. Kind of felt like a rubber band slightly snapping my skin. A green light blinked showing it worked. About 27 hours later, another beep was heard. It then administered the medicine and the green light flashed faster. About an hour later the green light turned red. When the light was red, that indicated it was time to be removed. Because it was difficult for me to reach behind my arm, my husband loosened the adhesive and pulled it off.

When I was given Neulasta, I was encouraged to take Claritin before and after chemotherapy. It really helped prevent leg and hip pain which was a side effect of Neulasta. Because the Neulasta built up the bone marrow and the greatest intensity of bone marrow was in the hip and upper leg area, it could cause severe pain. I’m grateful because I took the Claritin, I never had any pain from that. However, Claritin aggravated my sinuses. So after a while, I lessened my Claritin dose.
The last twelve chemotherapy treatments were weekly. Because Neulasta can only be used every two weeks, if my blood levels fell lower, I was not allowed to have Neulasta. There was another type of shot that could be administered weekly to help build bone marrow. When my blood levels fell lower during the last twelve treatments a few times, I received a shot. Claritin did not help the leg/hip pain with the shot. In fact, I experienced some pain in my legs and hips as a result of the shot.
I was given a color-coded calendar which helped keep track of when I had to get labs, have chemotherapy treatment or take any medication such as Claritin or steroids before and/or after treatment. The calendar really helped to keep the grueling schedule clearer.
Chemotherapy regimens vary depending on the type of cancer. In the next, post, I will share the regimen the IU Thymus Guru along with my local oncologist chose specifically for my situation. I will also explain how I felt during chemotherapy along with the side effects I experienced.
I want to thank you for coming along this journey.
I want to leave you with this thought. Hebrews 11:1 “Faith is the confidence that what we hope for will actually happen; it gives us assurance about things we cannot see.” (NLT) My faith is what kept me going many times when circumstances looked bad.




God Bless you Debbie, thank you for sharing your battle it explains so much and helps me to understand a bit better what you and others have and do go through. You are one of the strongest people I know….Thank you!